Stacy's Story
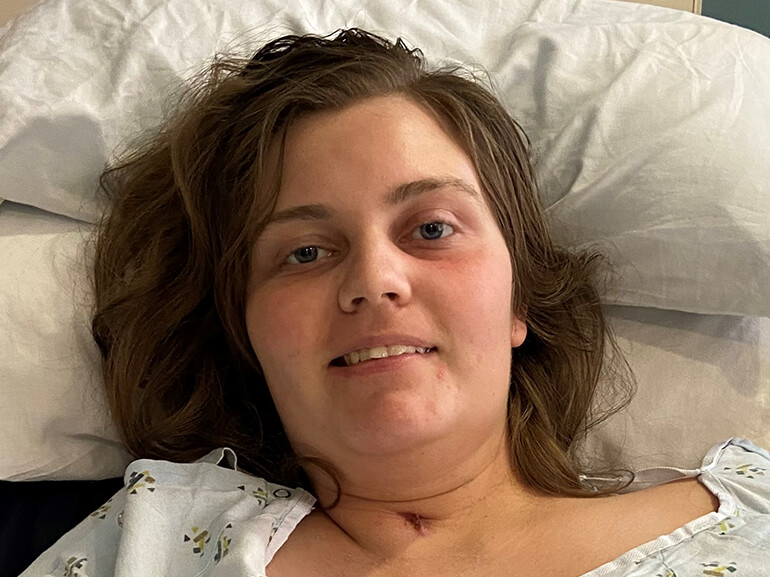
In July, Stacy Chavez and her husband, Raul, proudly welcomed their son, Noah.
The excitement of first-time parenthood gave way to concern as Stacy returned home and was plagued by headaches.
The pain intensified, her left arm growing numb and weak. Then, Stacy felt a seizure coming on and called for Raul to dial 911. He did, then helped her lay down until emergency crews arrived.
As the ambulance pulled up, Stacy had a second seizure and lost consciousness. Doctors stabilized the 25-year-old and immediately transferred her to a regional medical center in Oklahoma City. There, Raul learned his wife experienced a stroke due to bleeding on the brain.
She was placed on a ventilator, tracheostomy for airway support and feeding tube.
Raul’s mother stepped in to help with Noah and their hometown of Ada, Oklahoma, rallied behind the family. Residents hosted t-shirt sales, a catfish fry and started a Facebook page called “Chavez Strong” to raise money for her medical bills.
After 25 days, Stacy turned the corner. At the medical staff’s recommendation for extended healing, Raul had her transferred to Select Specialty Hospital – Oklahoma City.
Upon admission, Stacy was unconscious, unable to breathe, eat, speak or move independently. Raul hoped this next step of recovery would bring Stacy back to him and Noah.
A physician-led team, including nurses and therapists, created a plan to get make that happen.
Respiratory therapists collaborated with physicians to gradually reduce ventilator settings, allowing Stacy’s lungs to work independently.
Not long after, Stacy regained consciousness. Therapists started leading breathing and chest exercises to increase lung stamina. Stacy’s key turning point came several days later, when she felt alert enough to have a video chat with Raul and mouthed “I love you.”
Eventually, Stacy liberated from the ventilator. Speech and respiratory therapists coordinated to fit a valve into the airway support that allowed more normal speech.
Because COVID-19 restricted visitation, the care team coordinated regular video calls between Stacy and Raul. That’s when Stacy learned how her community had united to help her family.
“It’s amazing to see that people will come together and help someone they don’t even know,” she said.
That, coupled with her family’s support, provided powerful motivation to continue getting well.
Physical and occupational therapists led Stacy through arm, leg, hand and core exercises. They practiced standing and transitioning to a chair to build core strength. Occupational therapists retrained her on personal care skills, such as grooming and eating.
Stacy formed a special bond with the occupational therapist, who pushed her the hardest, but did everything with love. The therapist bought a book and wrote daily notes to Noah about Stacy’s strength and progress.
Meanwhile, speech therapists continued working on mouth, tongue and jaw exercises to rebuild throat muscles. When she could safely swallow food, the feeding tube was removed and dietitians designed a meal plan calibrated to provide healing nutrients and appropriate textures.
Sometimes, Stacy wondered why the stroke happened.
“I’ve asked God, and I think everything happens for a reason,” she said. “I learned I’m a lot stronger than I thought I was. If there’s one piece of advice I could give, it’s spend time with the people you love.”
After a month, Stacy was discharged to an inpatient rehabilitation hospital to continue building endurance and stability before returning home to Raul and Noah.