Frank’s Story
Compassionate care bridges the pandemic-driven divide
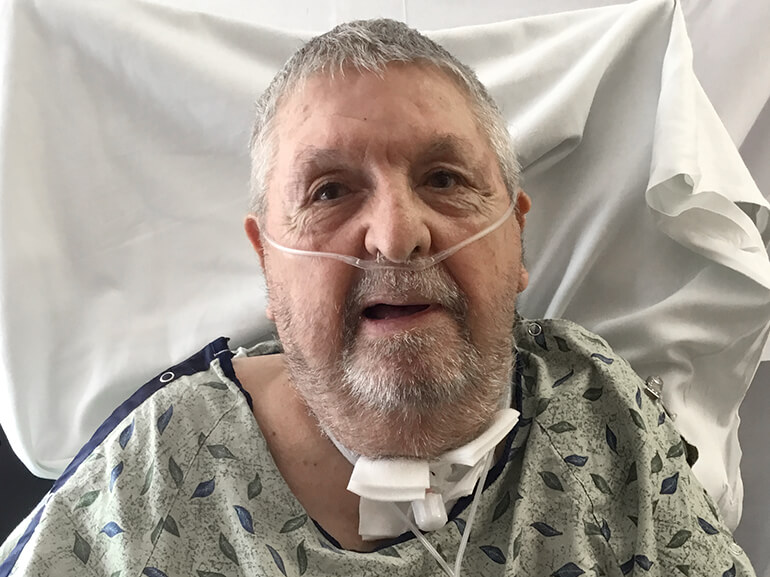
Everyone in Batesville, Indiana knows 87-year-old Frank Clark. Following a four-decade-long career at the local post office, he was a regular fixture at his grandchildren’s sporting events, the Veterans of Foreign Wars post and his porch, where he could be spotted socializing or sitting outside watching wildlife with his wife, Marti.
It’s an ease Frank fought hard to accomplish. He lost both parents to tuberculosis before age 10 and spent years in an orphanage and foster care. As a teenager, he worked as a farm hand, enlisting in the Army when he came of age. He transferred to the Air Force and while stationed in South Dakota, Frank also contracted tuberculosis losing a quarter of his lung to the disease.
In mid-March, as the COVID-19 pandemic spread across the United States, Marti came down with the virus. When Frank started feeling ill, daughters Molly and Amiee immediately took him to a clinic. Testing revealed low oxygen levels and a fever. Frank had COVID-19, too.
Admitted to his local hospital’s emergency room, then sent to Christ Hospital in Cincinnati, he spent the next 43 days fighting for his life. Doctors placed Frank on a ventilator and tracheostomy for airway support. Not long after, Marti was also hospitalized.
By the middle of May, the couple’s extended family had reason to celebrate. Marti had recovered and Frank stabilized. They chose Select Specialty Hospital – Cincinnati for the next step in Frank’s journey, due to its experience in ventilator liberation and complex coronavirus care.
Frank arrived unable to eat, breathe or move independently. Undaunted, he spent two months working with respiratory, physical, occupational and speech therapists to regain strength and stamina.
The respiratory team began by slowly reducing the amount of support Frank’s lungs received from the ventilator. They trialed short bursts of time off the machine. As he withstood longer periods, he liberated and speech therapists stepped in to place a valve in the airway support, allowing deeper breathing.
Eventually, Frank’s airway support was capped, permitting him to eat and communicate with family – something he dearly missed. The Cincinnati team arranged for regular video chats.
Speech therapists again stepped in, this time with exercises for his jaw, tongue and throat so Frank could safely swallow. Dietitians created a meal plan of pureed food to ease his transition back to regular meals.
Physical therapists and nursing staff ensured Frank was out of bed twice a day, sitting in a chair to help him rebuild core strength. Occupational therapy led grasping and pinching exercises to enhance dexterity.
As he grew stronger, physical therapists assisted Frank in standing up and fitted him with a rolling walker to take his first few steps since falling ill.
Soon, Frank could dress himself with minimal assistance and use a walker to travel the halls. Mobility, and a bit of socialization, perked Frank up even more. He progressed quickly, meeting his goals of moving, breathing, speaking and eating independently.
Because he still needed to build strength, Frank departed for an inpatient rehabilitation hospital, spending three hours each day focused on physical and occupational therapy.
By August, Frank had returned home, breathing independently. He’s back to enjoying the front porch with Marti, watching birds and animals hop through the yard.